
Colonic metastasis from primary lung adenocarcinoma: a case report and review of the literature
Introduction
Lung cancer has the highest cancer mortality rate in the United States (1). Non-small cell lung cancer, small cell lung cancer and lung carcinoid tumors are the three most prevalent lung cancers. About 85% of lung cancers are non-small cell lung cancers, which include the subtypes of adenocarcinoma, squamous cell carcinoma and large cell carcinoma (2). The most common sites of lung cancer metastasis are the adrenal glands, liver, bone and brain and the gastrointestinal (GI) system is rarely involved (3-7). The reported incidence of symptomatic GI metastasis is 0.2–0.5%, and generally it is not caught until an advanced stage (8). When the GI tract is involved, the small bowel is the most common site for metastasis. Metastasis to the colon is exceedingly rare and there are limited reports of this. Of the documented cases of lung cancer metastasis, fewer still involve the spread of adenocarcinoma. The most common type of lung tumor causing GI metastasis is squamous cell followed by large cell carcinoma. In Antler et al., adenocarcinoma only accounted for 8% of 423 autopsy cases of primary lung cancer metastasizing to the GI tract, showing its rarity (3). We present a case of primary lung adenocarcinoma that metastasized to the colon. Upon review of current literature only five such cases have been documented (4,8-11).
Case presentation
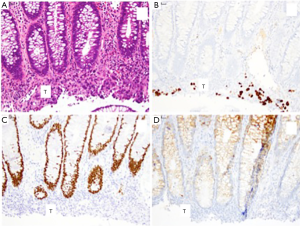
A 64-year-old man with a 41-pack-year history of smoking, emphysema and sleep apnea presented with hemoptysis in December 2014. A computerized tomography (CT) scan showed an ill-defined mass in the hilum of the right lung, mediastinal lymphadenopathy in the subcarinal region and an 8 mm nodule in the right upper lobe. There was scarring of the posterior right lower lobe and severe focal bullous emphysema. A full body positron emission tomography-computed tomography (PET/CT) scan in March 2015 revealed the additional findings of lymphadenopathy in the neck, 1 cm pancreatic lesion, multiple peritoneal tumor deposits, possible metastatic lesion and left femur mass. In April 2015 a fine needle aspiration on the left supraclavicular lymph node showed metastatic poorly differentiated non-small cell carcinoma, favoring adenocarcinoma. A colonoscopy revealed three non-cancerous polyps and an irregular area of mucosa of the splenic flexure. The biopsy of this area was inconclusive. The patient was therefore referred to Moffitt Cancer Center for a repeat colonoscopy and biopsy of the colon irregularity. At this time, the patient had rectal pain, but denied bleeding per rectum, nausea, vomiting and abdominal pain. He denied diarrhea and constipation, although was experiencing fecal urgency. The repeated biopsy of the colonic irregularity revealed an ulcerated colonic mucosa involved by a poorly differentiated metastatic adenocarcinoma consistent with primary lung adenocarcinoma (Figure 1A). The tumor was immunohistochemically positive for transcription factor 1 (TTF-1) (Figure 1B) and cytokeratin 7 (not shown) and negative for CDX2 (Figure 1C) and cytokeratin 20 (Figure 1D). The napsin immunostain was not contributory as the tumor was no longer present in the deeper section into the block.
Discussion
Primary lung adenocarcinoma metastasis to the colon is exceedingly rare. The most common metastatic site in the GI tract is the small bowel (4-7). Ryo et al. revealed that, in their study of 1,635 patients, GI metastasis of lung adenocarcinoma was 1.8%; 1.1% to small intestines, 0.4% to the stomach and 0.5% to the colon (12). Furthermore, most cases of primary lung cancer that metastasized to the GI were squamous cell carcinoma and large cell carcinoma, not adenocarcinoma. Antler et al. demonstrated that only 10% out of 58 cases of GI metastases were classified as adenocarcinoma (3). The exact incidence of adenocarcinoma metastases to the colon is unknown. Most publications found in the literature were isolated case reports, which highlight the rarity of this instance.
The patient we encountered had a past medical history significant for stage 4 adenocarcinoma of the lung. A PET/CT showed a mass in the colonic flexure. Subsequent immunohistochemistry staining of the colonic mass was positive for TTF-1 and CK-7, while being negative for CK-20 and CDX2. TTF-1 is commonly expressed in pulmonary epithelial cells, while CK-7 can be found in both pulmonary adenocarcinoma and upper GI or pancreatobiliary adenocarcinoma. CK-20 and CDX2 are markers commonly found in colonic adenocarcinoma (13-16). The positive TTF-1 and CK-7 stains support a pulmonary origin. The negative CK-20 and CDX2 markers mitigate against a colonic origin of the tumor. This conclusion is also supported by the absence of a premalignant colonic adenoma in the mucosa adjacent to the tumor.
The symptoms of a metastatic lung adenocarcinoma may be mistaken for the side effects of chemotherapy. This patient received two cycles of chemotherapy with carboplatin and pemetrexed with zometa for bone support, which could account for side effects such as weight loss, nausea, vomiting, diarrhea, constipation and weakness. Similar symptoms may be seen with primary or metastatic lung cancer to the colon. Lung cancer with intestinal metastasis has been reported to have a mean survival of only 4–8 weeks (17).
The patient reported experiencing weight loss, fecal urgency, and rectal pain. While none of these symptoms are particularly indicative for intestinal malignancies, in a patient with an advanced stage colon carcinoma, these symptoms should not be ignored. Because patients with lung cancer metastasis to the GI tract are often asymptomatic, manifestations of GI irregularity should be investigated further. It has been reported that about one third of lung cancer metastases to the colon are asymptomatic and found during an autopsy. The prevalence at autopsy of primary lung carcinoma metastasizing to the colon is about 4.7–14% (3,18). When symptomatic, the most common symptoms are abdominal pain, nausea, vomiting, anemia and weight loss (3,17,19).
Metastasis to the colon of primary lung adenocarcinoma is very rare. While documented cases do exist, a firm protocol of practice is still difficult to establish. However, through appropriate measures, positive patient outcomes can be achieved. Through the use of suitable immunohistochemical staining and screening using PET, an earlier diagnosis can be made allowing for improved quality and longevity of life. Because of the asymptomatic nature of this disease progression, recognizing symptoms of colonic metastasis is imperative to proper diagnosis.
Acknowledgements
Funding: None.
Footnote
Conflicts of Interest: The authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/amj.2017.01.19). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- U.S. cancer statistics working group. United States cancer statistics: 1999-2012 incidence and mortality web-based report. Atlanta GA: Department of Health and Human Services, Center for Disease Control and Prevention, and National Cancer Institute, 2015. Available online: http://www.cdc.gov/cancer/lung/basic_info/index.htm
- American Cancer Society. Lung cancer. January 2016. Available online: http://www.cancer.org/cancer/lungcancer/
- Antler AS, Ough Y, Pitchumoni CS, et al. Gastrointestinal metastases from malignant tumors of the lung. Cancer 1982;49:170-2. [Crossref] [PubMed]
- Weng MW, Wang HC, Chiou JC, et al. Colonic metastasis from a primary adenocarcinoma of the lung presenting with acute abdominal pain: a case report. Kaohsiung J Med Sci 2010;26:40-4. [Crossref] [PubMed]
- Yang CJ, Hwang JJ, Kang WY, et al. Gastro-intestinal metastasis of primary lung carcinoma: clinical presentations and outcome. Lung Cancer 2006;54:319-23. [Crossref] [PubMed]
- Yamamoto M, Matsuzaki K, Kusumoto H, et al. Gastric metastasis from lung carcinoma. Case report. Hepatogastroenterology 2002;49:363-5. [PubMed]
- Carroll D, Rajesh PB. Colonic metastases from primary squamous cell carcinoma of the lung. Eur J Cardiothorac Surg 2001;19:719-20. [Crossref] [PubMed]
- Gonzalez-Tallon AI, Vasquez-Guerrero J, Garcia-Mayor MA. Colonic Metastases From Lung Carcinoma: A Case Report and Review of the Literature. Gastroenterology Res 2013;6:29-33. [PubMed]
- Pezzuto A, Mariotta S, Fioretti F, et al. Metastasis to the colon from lung cancer presenting with severe hyponatremia and dyspnea in a young male: A case report and review of the literature. Oncol Lett 2013;5:1477-80. [PubMed]
- Huang YM, Hsieh TY, Chen JR, et al. Gastric and colonic metastases from primary lung adenocarcinoma: A case report and review of the literature. Oncol Lett 2012;4:517-20. [PubMed]
- Carson HJ, Eilers SG, Misra S. An unusual presentation of colonic metastasis of adenocarcinoma of the lung. Rev Esp Patol 2013;46:90-2. [Crossref]
- Ryo H, Sakai H, Ikeda T, et al. Gastrointestinal metastasis from lung cancer. Nihon Kyobu Shikkan Gakkai Zasshi 1996;34:968-72. [PubMed]
- Lau SK, Luthringer DJ, Eisen RN. Thyroid transcription factor-1: a review. Appl Immunohistochem Mol Morphol 2002;10:97-102. [Crossref] [PubMed]
- Matoso A, Resnick MB, Wang LJ. Comparison of 2 monoclonal TTF-1 antibodies. Appl Immunohistochem Mol Morphol 2011;19:384. [Crossref] [PubMed]
- Zhang PJ, Shah M, Spiegel GW, et al. Cytokeratin 7 immunoreactivity in rectal adenocarcinomas. Appl Immunohistochem Mol Morphol 2003;11:306-10. [Crossref] [PubMed]
- Chen ZM, Wang HL. Alteration of cytokeratin 7 and cytokeratin 20 expression profile is uniquely associated with tumorigenesis of primary adenocarcinoma of the small intestine. Am J Surg Pathol 2004;28:1352-9. [Crossref] [PubMed]
- Berger A, Cellier C, Daniel C, et al. Small bowel metastases from primary carcinoma of the lung: clinical findings and outcome. Am J Gastroenterol 1999;94:1884-7. [Crossref] [PubMed]
- McNeill PM, Wagman LD, Neifeld JP. Small bowel metastases from primary carcinoma of the lung. Cancer 1987;59:1486-9. [Crossref] [PubMed]
- John AK, Kotru A, Pearson HJ. Colonic metastasis from bronchogenic carcinoma presenting as pancolitis. J Postgrad Med 2002;48:199-200. [PubMed]
Cite this article as: Thomas K, Mirza Z, Coppola D, Friedman M. Colonic metastasis from primary lung adenocarcinoma: a case report and review of the literature. AME Med J 2017;2:12.

