Foreign body removal in children and adults: review of available techniques and emerging technologies
Foreign body aspiration is a considerable source of morbidity in adults and is the number one cause of death due to asphyxia in children, especially during first three years of life (1,2). Risk factors for foreign body aspiration in adults include conditions associated with compromised airway defenses and depressed level of consciousness such as alcohol intoxication, use of sedative and hypnotic medications and senility. Other risk factors include conditions associated with dysphagia, such as stroke and Parkinson’s disease, as well as esophageal motility disorders and gastrointestinal reflux disease (3). In children, natural curiosity during oral phase, as well as laughing, crying and playing during meals, is responsible for increased incidence of foreign body aspiration (4). The most frequently aspirated foreign body in adults is meat, although cultural and lifestyle variations play an important role in the diversity of aspirated materials in adults (5). The most common aspirated foreign bodies in children are peanuts (6).
Signs and symptoms of foreign body aspiration in adults are often nonspecific, requiring a clinician to maintain a high degree of clinical suspicion to establish a timely diagnosis. Clinical presentation depends on the type of foreign body and its location in the airway, the length of time between the aspiration event and diagnosis, and the host’s reaction to foreign body. A small object located near the vocal cords will result in significant cough while a larger object aspirated into distal bronchus may result in non-specific symptoms such as chronic cough and post obstructive pneumonia. Other common signs and symptoms of aspiration in adults include chronic cough, recurrent pneumonia, non-resolving wheezing, chest pain and hemoptysis (3). Up to 39% of patients with foreign body aspiration will have no physical findings resulting in a delay in diagnosis (7). Contrary to adults, the majority of children present with the penetration syndrome, defined as sudden onset of choking and cough shortly following aspiration. Owning to a more central location of aspirated object, as well as parental alertness, the time to diagnosis is typically shorter in children than adults (3).
Plain chest radiography, though an initial study of choice for suspected foreign body aspiration, may be normal as the majority of foreign bodies are radiolucent. Other radiographic signs include unilateral hyperinflation, atelectasis, mediastinal shift, pulmonary infiltrates and presence of radiopaque foreign bodies (3). In published studies, the diagnostic accuracy of plain films for detection of foreign bodies ranges between 40–70% (8). In children, the presence of pneumomediastinum and subcutaneous emphysema should alert clinicians to the possible presence of foreign body. Computerized tomography (CT) is helpful in detection of foreign bodies as well as demonstrating late complications of foreign body aspiration such as bronchial stenosis, bronchiectasis and post obstructive pneumonia.
The likelihood of tissue reaction to the aspirated foreign body depends on the content of foreign body and the length of time the foreign body remains in the airway. Peanuts are particularly irritating and often result in exuberant production of granulation tissue (9). Aspiration of pills presents a unique challenge as pills rapidly dissolve in the airway making their detection during bronchoscopy difficult. Local effects depend on chemical properties of an individual pill and duration of mucosal contact. Upon getting absorbed into bronchial mucosa, pills cause intense inflammation which may lead to granulation tissue and bronchial stenosis. Systemic effects from aspirated pill absorption across the mucosal surfaces have been described (10). Since many cases of pill aspiration do not reveal a foreign body at the time of bronchoscopic examination, endobronchial surveillance plays an important role in the timely identification and management of potential endobronchial complications.
Nonoperative techniques for management of foreign body aspiration, such as bronchodilator inhalation and postural drainage, are generally not recommended due to the risk of dislodgement and complete airway obstruction (11). Therapeutic percussion has met with mixed results. Bronchoscopy is the cornerstone for diagnosis and management of patients with foreign body aspiration. Comprehensive examination with flexible bronchoscopy is essential as foreign body may be covered with blood or granulation tissue and may be difficult to visualize. Success rate for removing foreign body depends on location, type of foreign body and operator experience. In experienced hands, flexible bronchoscopy can be successful in nearly 90% of cases of foreign body aspiration (12,13). Preference to add rigid bronchoscopy depends on local resources and expertise. In United States less than 10% of pulmonologists regularly perform rigid bronchoscopy and therefore flexible bronchoscopy remains the most commonly used approach for FB removal (14). Flexible bronchoscopy is also more convenient as it can be performed under light sedation without the need to utilize operating room resources. However, it is essential that every operator recognizes the limitations of flexible bronchoscopy and promptly refers patients to a tertiary center if expertise and facilities for foreign body removal, such as rigid bronchoscopy, are not available in a smaller institution.
Flexible tools for foreign body removal in adults are illustrated in Figure 1. Grasping forceps are most widely available and come in different designs. Rat tooth forceps are ideal for removing foreign objects with smooth surface where a firm grip is needed to prevent an object from slipping. Grasping forceps are not ideal for removing friable organic objects due to potential of fracture and dispersion of friable object into distal airways. Inflatable balloon catheters are a tool often underutilized by pulmonologists for retrieval of distally located foreign body. During the procedure the catheter is advanced distal to foreign body, the balloon is inflated and pulled proximally until the object is dislodged and its removal can be facilitated with the use of other available instruments. Magnet extractors consist of a flexible probe with a magnet cylinder on its tip. It is used for retrieval of mobile metallic objects. Occasionally surrounding granulation tissue must be cleared prior to attempting removal of a foreign body, which can be safely accomplished with electrocautery or laser.
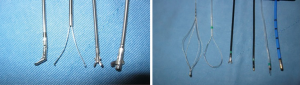
Since the majority of flexible bronchoscopic tools require a large working channel, there are far fewer tools available for pediatric populations compared with adults. Rigid bronchoscopy is therefore considered the standard of care for foreign body removal in pediatric populations and carries a success rate of over 90% (15). Rigid bronchoscopy also affords better airway control, better optics, and access to larger instruments. However there is now emerging data on the safety of foreign body removal with flexible bronchoscopy in the pediatric population. The use of a laryngeal mask (LMA) allows for insertion of a larger bronchoscope and access to multiple tools typically available to adult pulmonologist (16). Although the transition from rigid to flexible bronchoscopy is getting increasingly accepted in many medical centers, a multidisciplinary approach involving pediatric pulmonologists, ENT and thoracic surgeons is essential to ensure patient safety and maximize therapeutic success of the procedure.
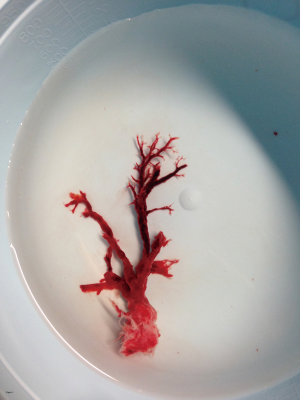
Cryotherapy is a novel technique for removing organic foreign bodies including mucous plugs and blood clots. Cryotherapy is based on Joule-Thomson principle, where sudden expansion of gas from a high pressure region to low pressure region results in cooling of the tip of the cryoprobe, allowing for freezing upon direct contact of the probe with tissue. This tissue adherence can be used to facilitate removal of foreign bodies. Figure 2 illustrates various components of the cryomachine. Cryoprobes are 90 cm in length and are available as 1.9 and 2.4 mm in outer diameter. Under bronchoscopic guidance, the tip of the cryoprobe is inserted inside the body of the lesion. Typical contact time between the probe and foreign body is 5–7 seconds. Because the foreign body is frozen to the tip of the cryoprobe, it is necessary to remove the cryoprobe en-bloc along with the bronchoscope. The foreign body typically detaches from the probe a few seconds after immersing the cryoprobe into warm water. Cryosensitivity of tissue depends on its intracellular water content and vascularity. Cartilage is cryoresistant, whereas granulation tissue, tumor and organic foreign bodies are cryosensitive. Although it is generally accepted that cryoextraction works best for organic foreign bodies, there may be a role for removing smaller inorganic foreign bodies devoid of water content, especially when the inorganic foreign body is coated with saline (17). One of cryotherapy’s most cited applications is removing obstructive blood clots in patients with massive hemoptysis, a procedure that is often difficult and time consuming when performed with standard flexible bronchoscopy alone (Figure 3) (18-20). Cryotherapy in the central airway has a favorable safety profile. Cryotherapy avoids cryoresistant cartilage and confers no risk of airway fire hence obviating the need to reduce inspired fraction of oxygen. Bronchoscopists must exercise caution to avoid contact between cryoprobes and surrounding mucosa. Other applications of cryotherapy include tumor debulking, treatment of carcinoma in situ in the central airways, and transbronchial cryobiopsies for interstitial lung disease (21).
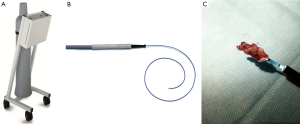
Cryotherapy has also successfully been used to facilitate removal of foreign bodies via flexible bronchoscopy in children younger than 40 months of age (22,23). Although a 1.9 mm cryoprobe is too large to fit down a pediatric bronchoscope’s 1.2 mm working channel, a new hybrid bronchoscope from Olympus (BF-MP 160) combines a pediatric 4.0 mm outer diameter with an adult size 2.0 mm working channel that accommodates cryoprobe and most adult size flexible tools used for foreign body extraction. Most authors recommend shortening freezing time to 2–4 seconds in pediatric population to avoid trauma to nearby tissues. Although cryotherapy through a flexible bronchoscope and LMA has been shown to be an effective technique in foreign body removal in the pediatric population, it is not currently the standard of care and further studies are required on safety and efficacy of such approach.
There is ongoing debate over the preferred method of administration of anesthesia for foreign body removal. Moderate sedation affords preservation of cough reflex which can facilitate foreign body removal. However critics of this approach raise concerns about losing the foreign body in the central airway, resulting in asphyxiation. Such complication has not been reported in the literature and endotracheal intubation can always be performed to secure the airway. In patients in whom the foreign body is too large to be removed through the endotracheal tube, the tube should be removed in conjunction with the bronchoscope. In children it is generally recommended to maintain spontaneous ventilation and remove foreign bodies with the use of rigid bronchoscope (24).
Complications of foreign body aspiration can be divided into acute and chronic. Acute complications include asphyxia and respiratory failure from central airway obstruction. Long-term complications include pneumonia, atelectasis and empyema. Complications that can occur during removal of foreign body include bleeding, pneumothorax and rupture of tracheobronchial tree. Timely recognition of foreign body aspiration and a multidisciplinary approach including the availability of rigid bronchoscopy can help reduce these complication rates. Significant hemoptysis associated with foreign body removal is rare and can often be controlled with instillation of dilute epinephrine, cold saline and coagulation of mucosa with endobronchial electrocautery (25). Complication rates are higher during foreign body removal in children. In a large series of pediatric patients with mean age of 4.1 years, the complication rate was up to 14% (26). Failure to grasp foreign body with proper forceps, swelling of organic objects caused by absorption of moisture and a small internal diameter of child’s tracheobronchial tree contribute to higher complications rates during foreign body removal seen in children (27).
Acknowledgements
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Amit Mahajan, Sandeep J. Khandhar and Erik E. Folch) for the series “Management of Complex Airway and Pleural Diseases” published in AME Medical Journal. The article has undergone external peer review.
Conflicts of Interest: The author has completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/amj.2018.07.02). The series “Management of Complex Airway and Pleural Diseases” was commissioned by the editorial office without any funding or sponsorship. The author has no other conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Baharloo F, Veyckemans F, Francis C, et al. Tracheobronchial foreign bodies: presentation and management in children and adults. Chest 1999;115:1357-62. [PubMed]
- Eren S, Balci AE, Dikici B, et al. Foreign body aspiration in children: experience of 1160 cases. Ann Trop Paediatr 2003;23:31-7. [Crossref] [PubMed]
- Folch E, Majid A. Bronchoscopy for Foreign Body Removal. In: Mehta A, Jain P, editors. Interventional Bronchoscopy. Respiratory Medicine. Totowa, NJ: Humana Press 2013, vol 10.
- Marquette CH, Martinot A. Interventinal bronchoscopy, Basel: Karger; 2000.
- Mittleman RE, Wetli CV. The fatal cafe coronary. Foreign-body airway obstruction. JAMA 1982;247:1285-8. [Crossref] [PubMed]
- Aziz F. Natural History of an Aspirated Foreign Body. J Bronchology Interv Pulmonol 2006;13:161-2.
- McGuirt WF, Holmes KD, Feehs R, et al. Tracheobronchial foreign bodies. Laryngoscope 1988;98:615-8. [Crossref] [PubMed]
- Martinot A, Closset M, Marquette CH, et al. Indications for flexible versus rigid bronchoscopy in children with suspected foreign-body aspiration. Am J Respir Crit Care Med 1997;155:1676-9. [Crossref] [PubMed]
- Haddadi S, Marzban S, Nemati S, et al. Tracheobronchial Foreign-Bodies in Children; A 7 Year Retrospective Study. Iran J Otorhinolaryngol 2015;27:377-85. [PubMed]
- Küpeli E, Khemasuwan D, Lee P, et al. "Pills" and the air passages. Chest 2013;144:651-60. [Crossref] [PubMed]
- Bose P, El Mikatti N. Foreign bodies in the respiratory tract. A review of forty-one cases. Ann R Coll Surg Engl 1981;63:129-31. [PubMed]
- Surka A, Bowling MR, Chin R, et al. Bronchoscopic Myths and Legends: Bronchoscopy in the Treatment of Lobar Atelectasis. Clin Pulm Med 2007;14:302-5. [Crossref]
- Swanson KL, Prakash U, McDougall JC, et al. Airway Foreign Bodies in Adults. J Bronchology Interv Pulmonol 2003;10:107-11.
- Prakash UB, Offord KP, Stubbs SE. Bronchoscopy in North America: the ACCP survey. Chest 1991;100:1668-75. [Crossref] [PubMed]
- Boufersaoui A, Smati L, Benhalla KN, et al. Foreign body aspiration in children: experience from 2624 patients. Int J Pediatr Otorhinolaryngol 2013;77:1683-8. [Crossref] [PubMed]
- Tenenbaum T, Kähler G, Janke C, et al. Management of Foreign Body Removal in Children by Flexible Bronchoscopy. J Bronchology Interv Pulmonol 2017;24:21-8. [Crossref] [PubMed]
- Wellikoff A, Tindel S, Kanitker A, et al. Aspirated Metallic Foreign Body Extraction Using a Flexible Cryoprobe. Chest J 2011;140:160A. [Crossref]
- Sehgal IS, Dhooria S, Agarwal R, et al. Use of a Flexible Cryoprobe for Removal of Tracheobronchial Blood Clots. Respir Care 2015;60:e128-31. [Crossref] [PubMed]
- Weerdt SD, Noppen M, Remels L, et al. Successful Removal of a Massive Endobronchial Blood Clot by Means of Cryotherapy. J Bronchology Interv Pulmonol 2005;12:23-4.
- Sriratanaviriyakul N, Lam F, Morrissey BM, et al. Safety and Clinical Utility of Flexible Bronchoscopic Cryoextraction in Patients With Non-neoplasm Tracheobronchial Obstruction: A Retrospective Chart Review. J Bronchology Interv Pulmonol 2015;22:288-93. [Crossref] [PubMed]
- DiBardino DM, Lanfranco AR, Haas AR. Bronchoscopic Cryotherapy. Clinical Applications of the Cryoprobe, Cryospray, and Cryoadhesion. Ann Am Thorac Soc 2016;13:1405-15. [Crossref] [PubMed]
- Zhang L, Yin Y, Zhang J, et al. Removal of foreign bodies in children's airways using flexible bronchoscopic CO2 cryotherapy. Pediatr Pulmonol 2016;51:943-9. [Crossref] [PubMed]
- Kazachkov M, Vicencio A. Foreign body removal is getting "cooler". Pediatr Pulmonol 2016;51:886-8. [Crossref] [PubMed]
- Fidkowski CW, Zheng H, Firth PG. The anesthetic considerations of tracheobronchial foreign bodies in children: a literature review of 12,979 cases. Anesth Analg 2010;111:1016-25. [PubMed]
- Rees JR. Massive hemoptysis associated with foreign body removal. Chest 1985;88:475-6. [Crossref] [PubMed]
- Hasdiraz L, Oguzkaya F, Bilgin M, et al. Complications of Bronchoscopy for Foreign Body Removal: Experience in 1035 Cases. Ann Saudi Med 2006;26:283-7. [Crossref] [PubMed]
- Tahir N, Ramsden WH, Stringer MD. Tracheobronchial anatomy and the distribution of inhaled foreign bodies in children. Eur J Pediatr 2009;168:289-95. [Crossref] [PubMed]
Cite this article as: Shostak E. Foreign body removal in children and adults: review of available techniques and emerging technologies. AME Med J 2018;3:75.