
Main d’accoucheur (obstetrician’s hand) after thyroidectomy: a video-illustrated case report
Introduction
Current medical teaching requires modern educational material. We report herein the case of a patient with Chvostek’s and Trousseau’s signs. These signs of hypocalcemia are presented with high-quality videos and images and were found on postoperative day (POD) one after total thyroidectomy.
Case presentation
A 34-year-old patient was referred to our surgical consultation for tachycardia with sporadic palpitations, frequent diarrheas, and ophthalmopathy (exophthalmos and intermittent diplopia). Laboratory tests found increased levels of triiodothyronine (T3) and thyroxine (T4), very low levels of thyroid-stimulating hormone (TSH, thyrotropin), and positive thyroid-stimulating antibodies. Ultrasound examination confirmed a diffusely enlarged thyroid gland. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this Case Report and any accompanying images/videos.
The diagnosis of Graves disease (also known as toxic diffuse goiter or Basedow disease) was made. The patient had no past medical history and took no specific medication. Family and psychosocial histories were without particularities.
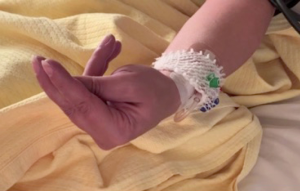
The patient therefore underwent total thyroidectomy by cervicotomy. No intraoperative complications occurred. All four parathyroid glands were intraoperatively visualized and preserved during dissection. On POD one her corrected calcium level lowered to 1.7 mmol/L (normal range: 2.1–2.6 mmol/L). At that time, the patient did not mention any symptoms (in particular peri-oral or digital paresthesias) but presented positive Chvostek’s sign (Video 1) and Trousseau’s sign (main d’accoucheur, obstetrician’s hand, Figure 1 and Video 2) on physical examination.
To summarize, the patient’s first consultation with her general practitioner was approximately two months before the surgical consultation, where investigations were undertaken and diagnosis of Graves disease was made. Total thyroidectomy was therefore scheduled one week after all investigations were terminated. Hypocalcemia symptoms appeared on POD one and treatment with IV calcium was directly initiated. Patient was discharged on POD two.
Discussion
These two signs are classical manifestations of hypocalcemia due to neuronal hyperexcitability. Chvostek’s sign (Video 1) is defined as a spasm of the ipsilateral orbicularis oris after percussion of the facial nerve area (the region anterior to the ear tragus) (1). This sign was first described by a Viennese surgeon, born in Czech Republic, named František Chvostek in 1876. This test is useful in case of clinical suspicion of hypocalcemia. It has a sensitivity of 29% and a specificity of 75% (2).
When inflating the sphygmomanometer cuff above the patient’s systolic pressure induces hand muscle tetany (wrist and metacarpophalangeal joint flexion with interphalangeal joint extension, main d’accoucheur, French for obstetrician’s hand), it is known as Trousseau’s sign (Figure 1 and Video 2) (3). Dr. Armand Trousseau, a French physician, described this clinical sign in 1861. Trousseau’s sign is more sensitive and specific (around 90%), and more precocious than Chvostek’s sign in case of hypocalcemia (1). Chvostek’s sign and Trousseau’s sign can be found in up to 25% and 4% of healthy adults with normal blood calcium levels, respectively (1,4,5).
Hypocalcemia is a common complication after total thyroidectomy (around 10%) and is due to a postoperative hypoparathyroidism (6). Hypocalcemia can be transitory (in around 80–85% of cases of hypocalcemia) or persistent (in around 15–20%) (6). It is presently not clear when and how many times serum calcium should be measured postoperatively after total thyroidectomy. The actual trend tends towards diminishing the number of laboratory tests and focusing on the symptomatology and clinical examination of the patients. In our institution corrected and total calcium levels are measured 6 hours after total thyroidectomy and on POD one unless hypocalcemia-related symptomatology or positive presence of Trousseau’s or Chvostek’s signs appear. Presence of hypocalcemia symptoms or signs mandates oral or intravenous calcium substitution.
The patient hypocalcemia was substituted with IV calcium gluconate and oral calcium with good tolerance and compliance after explanation of the risks if left untreated. No adverse nor unanticipated events were found during treatment. The calcemia rapidly normalized and Chvostek’s and Trousseau’s signs concomitantly resolved. The patient was discharged home on POD two with oral calcium supplementation. A follow-up consultation was scheduled with an endocrinologist one month after the operation.
The strength of this article is the high-quality educational material illustrating the signs of hypocalcemia, which can be found in Graves disease (as in this case) or in other causes inducing low blood calcium level. A limitation of our manuscript is that a single report of a case precludes generalization of the findings.
As a take home message, clinical signs such as Trousseau’s or Chvostek’s signs are easily and rapidly performed bedside on the contrary of laboratory and imaging tests. Clinical investigation should remain the cornerstone of medical practice.
Conclusions
Chvostek’s and Trousseau’s signs are important clinical signs to seek after total thyroidectomy. They can be the first signs of calcium deficiency and can therefore help to make the diagnosis of hypocalcemia sooner.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at https://amj.amegroups.com/article/view/10.21037/amj-2020-03/coif). GRJ serves as an unpaid editorial board member of AME Medical Journal from February 2020 to February 2022. The other author has no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this Case Report and any accompanying images/videos. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Jesus JE, Landry A. Images in clinical medicine. Chvostek’s and Trousseau’s signs. N Engl J Med 2012;367:e15. [Crossref] [PubMed]
- Ahmed S, Saeed F, Rahman F. Severe isolated primary hypoparathyroidism in an adult. J Coll Physicians Surg Pak 2011;21:111-2. [PubMed]
- Meininger ME, Kendler JS. Images in clinical medicine. Trousseau’s sign. N Engl J Med 2000;343:1855. [Crossref] [PubMed]
- Page C, Strunski V. Parathyroid risk in total thyroidectomy for bilateral, benign, multinodular goitre: report of 351 surgical cases. J Laryngol Otol 2007;121:237-41. [Crossref] [PubMed]
- Sturniolo G, Lo Schiavo MG, Tonante A, et al. Hypocalcemia and hypoparathyroidism after total thyroidectomy: a clinical biological study and surgical considerations. Int J Surg Investig 2000;2:99-105. [PubMed]
- Bergenfelz A, Jansson S, Kristoffersson A, et al. Complications to thyroid surgery: results as reported in a database from a multicenter audit comprising 3,660 patients. Langenbecks Arch Surg 2008;393:667-73. [Crossref] [PubMed]
Cite this article as: Gaspar Figueiredo S, Joliat GR. Main d’accoucheur (obstetrician’s hand) after thyroidectomy: a video-illustrated case report. AME Med J 2020;5:32.

